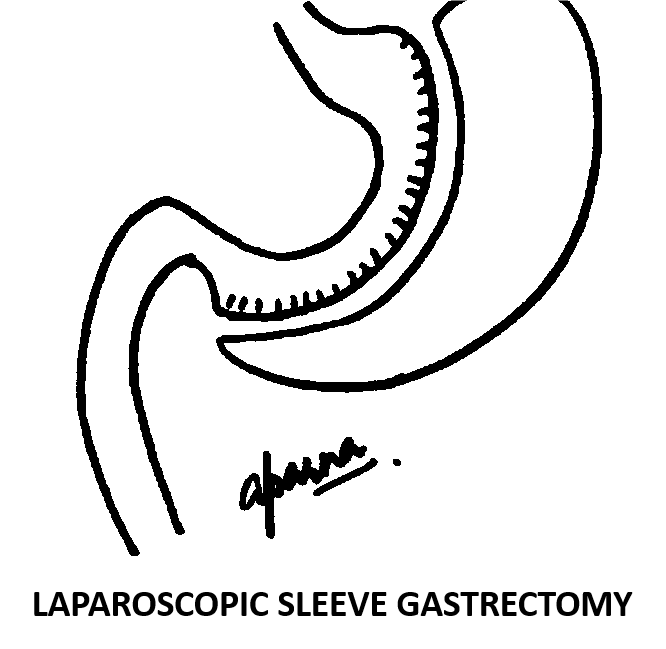
Laparoscopic Sleeve Gastrectomy- Frequently asked questions
Laparoscopic sleeve gastrectomy is a type of weight loss surgery/bariatric surgery. As the name suggests it can be performed through key-hole method (laparoscopy). In this technique 4 to 5 tiny cuts of half to one cm are made on the abdomen and the whole surgery is performed through these. Laparoscopic sleeve gastrectomy can also be performed in the scar-less manner through a single cut through the belly button. In this procedure, the stomach is divided longitudinally using surgical staplers and two-thirds of the stomach is removed. This results into a banana shaped stomach with a capacity of 60 to 100 cc.
FAQs (Frequently asked questions)
- Who is eligible for laparoscopic sleeve gastrectomy?
Following are the criteria for eligibility-
- BMI ≥5 Kg/m2 with or without associated diseases
- BMI ≥5 Kg/m2 with 2 or more associated diseases like type 2 diabetes, high blood pressure, sleep apnoea etc.
- BMI ≥5 Kg/m2 with uncontrolled diabetes despite best medical management
- Who must not undergo laparoscopic sleeve gastrectomy?
- Patients suffering from severe acidity, reflux disease or hiatus hernia
- Patients with gastric outlet obstruction
- Smokers
- Patients who are pregnant or wish to be pregnant in the next 1 year
- Patients who are medically unfit for any kind of surgery
- Patients with severe uncontrolled psychiatric disorders
- What kind of weight loss can be achieved after a laparoscopic sleeve gastrectomy?
Laparoscopic sleeve gastrectomy is a primarily restrictive procedure and can lead to an excess weight loss of about 65 to 75% on an average. This occurs over a period of 12 to 18 months. Various factors affect weight loss after bariatric surgery. It is important to recognize that obesity is a chronic progressive disease and needs life long support. Diet and lifestyle modification are mandatory after bariatric surgery to get good results and for weight maintenance.
- What are the risks associated with laparoscopic sleeve gastrectomy? Can I die in surgery? Will I become weak or bedridden after surgery?
Laparoscopic sleeve gastrectomy is as safe as any other surgery like gall bladder surgery or a knee replacement surgery. The overall risk of complications is less than 1%. Many complications like leak from staple lines, deep vein thrombosis and to the extent of death are listed on the web. It is important to visit a bariatric surgeon and understand the pros and cons and not just rely on hearsay and information on google. Regular follow up along with diet and behaviour modification is the key to long term success after bariatric surgery. There should be no weakness after the initial few weeks of surgery. If you continue to feel weak then you must get in touch with the bariatric team for further evaluation.
- Can I get cancer after a laparoscopic sleeve gastrectomy?
Acid reflux is a known complication after a laparoscopic sleeve gastrectomy. Studies have shown that 18 to 20% of patients may develop acid reflux or Barrette’s esophagus at the end of 5 years after a sleeve gastrectomy. However, till date, out of millions of patients who have undergone a laparoscopic sleeve gastrectomy only 1 or 2 cases of cancer in the esophagus have been reported. Yearly upper GI endoscopy is recommended after sleeve gastrectomy to check for any signs of reflux, ulcers or barrette’s esophagus.
Dr. Aparna Govil Bhasker is a Bariatric and Advanced Laparoscopic Surgeon.
Affiliations: Global Hospital, Parel; Apollo Hospitals, CBD Belapur, Tradeo and Chembur; Currae Hospital, Thane; Suchak hospital, Malad and Namaha Hospital, Kandivali
Mobile: +919819566618
Email: draparnagovil@gmail.com
Website: www.bestbariatricsurgeon.org