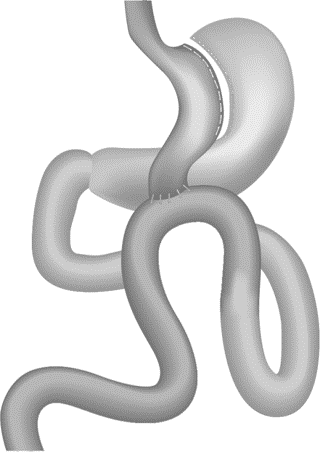
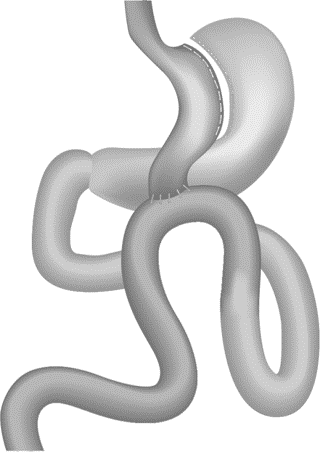
Laparoscopic mini gastric bypass is a type of weight-loss/bariatric surgery. As the name suggests it can be performed through key-hole method (laparoscopy). In this technique 4 to 5 tiny cuts of half to one cm are made on the abdomen and the whole surgery is performed through these. In a Laparoscopic mini gastric bypass, a long narrow stomach pouch is created using surgical staplers. A 150 to 200 cm loop of small intestine is then taken and attached to the stomach pouch in a loop fashion. The food comes into the stomach pouch and flows directly into the distal small intestine. It bypasses the remaining stomach and the first part of small intestine.
Laparoscopic mini gastric bypass surgery in mumbai leads to weight loss by various mechanisms. First of all, it leads to restriction of food intake. After a mini gastric bypass, the stomach pouch can hold lesser amount of food at one go. This reduces the amount of food that a person can have. As the stomach size is small, it also leads to feeling full sooner. The feeling of satiety sets in after eating even small quantities of food. After a Laparoscopic mini gastric bypass “hunger” sensation goes down significantly. This happens because the part of the stomach that is bypasses contains almost 80% of the hunger hormone called “ghrelin”. As the food does not come in contact with this part of the stomach, for the first year, most patients do not experience “hunger”. Hence, they are satisfied even after eating less food which is unlike being on a diet where one is constantly battling hunger and cravings. As the food also passes into the intestines faster than usual and this sets of a hormonal cascade that also aids in weight loss as well as helps in remission of type 2 diabetes. A mini gastric bypass is more mal-absorptive than a Roux en y gastric bypass. Ofcourse, there are other mechanisms like bile acid interactions and role of gut microbes. Alongwith these there are some unknown mechanisms and all of these when put together lead to weight loss after mini gastric bypass.
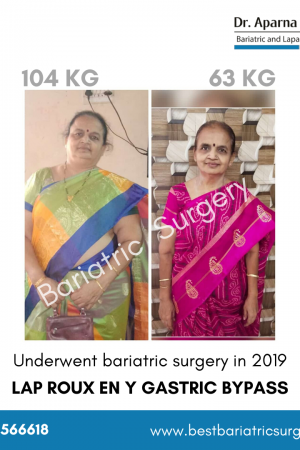
Laparoscopic mini gastric bypass leads to an excess weight loss of about 75 to 85% in 12 to 18 months. Patients also experience significant improvement in associated diseases like type 2 diabetes, high blood pressure, dyslipidemia, gout, PCOD, obstructive sleep apnoea, joint pains, liver disease etc. It also reduces the risk of venous thrombo-embolism and heart disease in the long term. Laparoscopic Roux en-y gastric bypass leads to a significant improvement in the quality of life of the patient.
In the long term the main issues observed with a laparoscopic mini gastric bypass are possible nutritional deficiencies and some degree of weight regain. However, obesity is a chronic progressive disease and as with any weight loss procedure, regular follow up with the bariatric team is the key to success after a laparoscopic mini gastric bypass. It is extremely important to follow a healthy lifestyle and a good exercise regime after a Laparoscopic mini gastric bypass. One must be very diligent with nutritional supplements and they must be taken as advised by the bariatric team. After an MGB, patients are prone to develop protein, calcium, vitamin and iron deficiencies. Hence it is important to be on life-long supplements to avoid these issues.
Bariatric Surgery/Obesity Surgery/ Weight Loss Surgery in india Patients Before After Photos
Dr. Aparna Govil Bhasker is a Bariatric Surgeon in Mumbai and Advanced Laparoscopic Surgeon.
Affiliations: Global Hospital, Parel; Apollo Hospitals, CBD Belapur, Tardeo and Chembur; Currae Hospital, Thane; Suchak hospital, Malad and Namaha Hospital, Kandivali; Belle Vue Hospital, Andheri West for Bariatric Surgery, Hernia Surgery and Gallbladder Surgery etc.
Mobile: +91 9819566618
Email: draparnagovil@gmail.com
Website: www.bestbariatricsurgeon.org